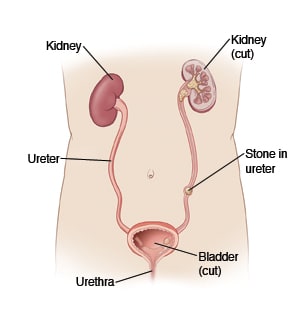
The sharp cramping pain on either side of your lower back and nausea or vomiting that you have are because of a small stone that has formed in the kidney. It's now passing down a narrow tube (ureter) on its way to your bladder. Once the stone reaches your bladder, the pain will often decrease. But it may come back as the stone continues to pass out of the bladder and through the urethra. The stone may pass in your urine stream in one piece. The size may be 1/16 inch to 1/4 inch (1 mm to 6 mm). Or the stone may break up into sandy-like fragments that you may not even notice.
Once you have had a kidney stone, you may be at risk of getting another one in the future. There are four types of kidney stones. Eighty percent are calcium stones, mostly calcium oxalate but also some with calcium phosphate. The other three types include uric acid stones, struvite stones (from a preceding infection) and, rarely, cystine stones.
Most stones will pass on their own. But they may take from a few hours to a few days. Sometimes the stone is too large to pass by itself. In that case, the doctor will need to use other ways to remove the stone. These methods include:
- Shock wave lithotripsy. This noninvasive procedure uses high energy sound waves to break up the stone and allow it to easily pass.
- Ureteroscopy. This procedure inserts a tool through the urethra and bladder and into the ureter to pull out the stone. This procedure is done under anesthesia.
- Surgery. You may need surgery to remove the stone.
Home care
The following are general care guidelines:
- Drink plenty of fluids. This means at least 12, 8-ounce glasses of fluid—mostly water—a day.
- Each time you pee (urinate), do so in a jar. Pour the urine from the jar through the strainer and into the toilet. Continue doing this until 24 hours after your pain stops. By then, if there was a kidney stone, it should pass from your bladder. Some stones dissolve into sand-like particles and pass right through the strainer. In that case, you won't ever see a stone.
- Save any stone that you find in the strainer and bring it to your doctor for a detailed exam. It may be possible to stop certain types of stones from forming. For this reason, it's important to know what kind of stone you have.
- Try to stay as active as possible. This will help the stone pass. Don't stay in bed unless your pain keeps you from getting up. You may notice a red, pink, or brown color to your urine. This is normal while passing a kidney stone.
- If you develop pain, you may take ibuprofen or naproxen for pain, unless another medicine was prescribed. Talk with your doctor before using these medicines if you have chronic liver or kidney disease. Or if you've had a stomach ulcer or digestive bleeding.
Preventing stones
Each year for the next 5 to 7 years, you are at risk that a new stone will form. Your risk is a 50% chance over this time period. The risk is higher if you have a family history of kidney stones or have certain chronic illnesses like high blood pressure, obesity, or diabetes. Making changes to your lifestyle and diet may lower your risk for another stone.
Most kidney stones are made of calcium. The following is advice for preventing another calcium stone. If you don't know the type of stone you have, follow this advice until the cause of your stone is found.
Things that help:
- The most important thing you can do is to drink plenty of fluids each day. See home care above.
- Eat foods that contain phytates. These include wheat, rice, rye, barley, and beans. Phytates are substances that may lower your risk for any type of stone to form.
- Eat more fruits and vegetables. Choose those that are high in potassium.
- Eat foods high in natural citrate, such as fruit and low-sugar fruit juices, such as lemon juice. Citrate can protect against kidney stones because it stops crystals from turning into stones.
- Having too little calcium in your diet can put you at risk for calcium kidney stones. Eat a normal amount of calcium in your diet and talk with your doctor if you are taking calcium supplements. Cutting back on your calcium intake may raise your risk. New research shows that eating calcium-rich and oxalate-rich foods together lowers your risk for stones by binding the minerals in the stomach and intestines before they can reach the kidneys.
- Limit salt intake to 2 grams (1 teaspoon) per day. High sodium in your diet will increase the amount of calcium sent into your urine. This can increase your chances of developing another stone. Use limited amounts when cooking, and don't add salt at the table. Processed and canned foods are usually high in salt.
- Spinach, rhubarb, peanuts, cashews, almonds, grapefruit, and grapefruit juice are all high-oxalate foods. You should limit how much of these you eat or eat them with calcium-rich foods. These include dairy products, dark leafy greens, soy products, and calcium-enriched foods.
- Reducing the amount of animal meat, shellfish, and high protein foods in your diet may lower your risk for uric acid stones. These foods have high amounts of a natural chemical compound called purines. Eating a lot of food with purines can make your body produce more uric acid. Limiting alcohol is also recommended to decrease uric acid production.
- Limit the amount of sugar (sucrose) and soft drinks with fructose in your diet.
- If you take vitamin C as a supplement, don't take more than 1,000 mg a day.
- A dietitian or your doctor can give you information about changes in your diet that will help prevent more kidney stones from forming.
Follow-up care
Follow up with your doctor as advised if the pain lasts more than 48 hours. Talk with your doctor about urine and blood tests to find out the cause of your stone. If you had an X-ray, CT scan, or other diagnostic test, you will be told of any new findings that may affect your care.
Call 911
Call
- Weakness, dizziness, or fainting.
When to get medical care
Contact your doctor right away if any of these occur:
- Pain that is not controlled by the medicine given
- Repeated vomiting or unable to keep down fluids
- Fever of
100.4 ºF (38 ºC) or higher, or as advised by your doctor - Passage of solid red or brown urine (can't see through it) or urine with lots of blood clots
- Foul-smelling or cloudy urine
- Unable to pee for 8 hours and increasing bladder pressure


